You hear the word “interoperability” used a lot these days in healthcare. But the word means different things to different people across the healthcare ecosystem. For clinicians, it may mean the ability to easily and quickly share unstructured data, such as x-ray images, while to another provider it might mean ensuring optimal patient care. For healthcare leadership, it may mean complying with regulations and effortlessly accessing a wide range of data across the organization to more effectively inform business decisions. And payers or insurers may want to see all inpatient, outpatient, pharmacy, and enrollment data in one place to help improve and speed up decision making processes.
To better understand the state of interoperability today, Snowflake partnered with Fierce Healthcare to survey a segment of healthcare providers, systems, regulators, and payers to ask about present-day challenges associated with interoperability as well as what they think interoperability can address. The survey revealed interesting insights, especially when comparing differences by job title, organization type, and role within the organization.
A couple of select findings from the report:
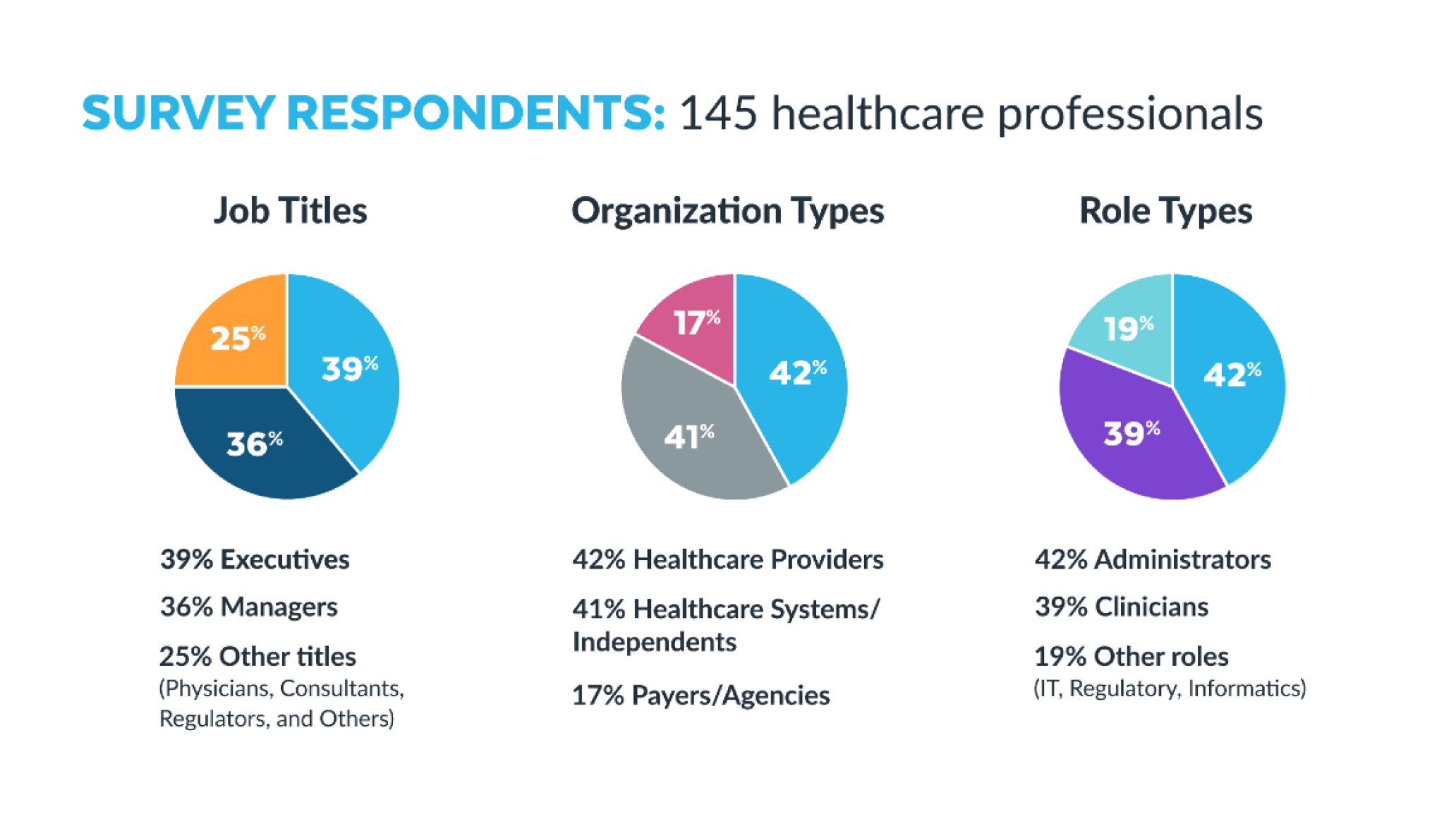
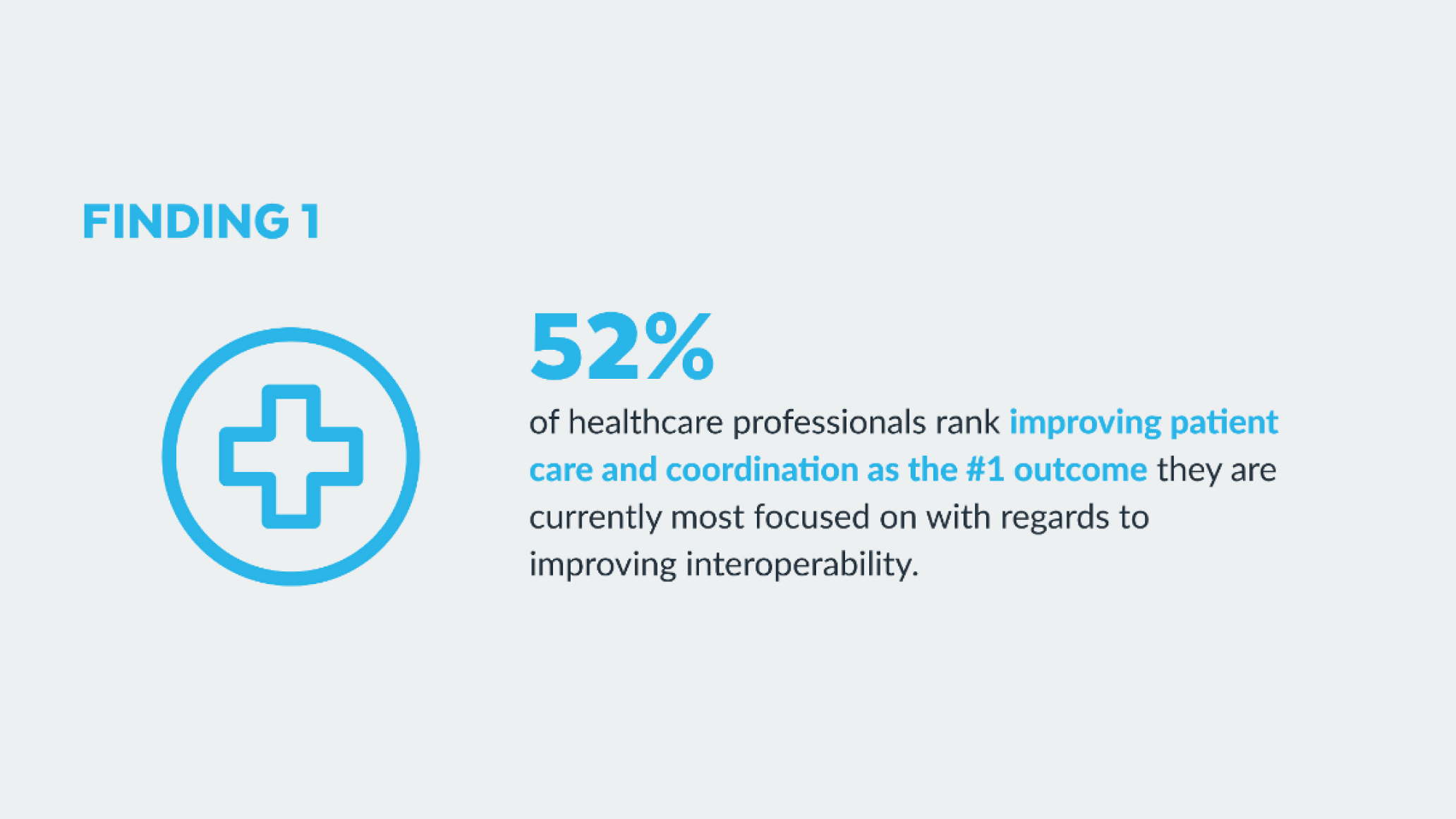

As the report indicates, the state of interoperability in healthcare is complex. A wide variety of technologies, data security concerns, and strict regulations guarding patient privacy impact the industry’s appetite for and ability to bring data together to improve outcomes. But perspectives about data sharing across the industry are changing, driven in large part by the recent pandemic.
At the onset of COVID, clinicians, healthcare providers, and payers shifted the majority of their work onto virtual platforms and other digital technologies practically overnight to care for patients. The result: the critical need to bring systems together to track and exchange data easily and effectively came to the forefront, driving further digital transformation and the need for improved interoperability. Without them, a complete view of the patient and their care journey was nearly impossible to achieve or very time-consuming to put together—undermining care quality. COVID also forced healthcare organizations to compile large amounts of data to analyze trends in infection, recovery, and death rates based on demographic, country, social determinants of health data, and more.
Timely, accurate data is essential to enabling optimal patient care, but data silos across the organization and legacy technologies make it nearly unattainable. And its impacts are noticeable. A recent industry report found that only “14% of healthcare executives are satisfied with the current accuracy of their patient/member profiles” and “72% of healthcare executives agree that siloed, inaccurate patient/member data is detrimental to care quality and business outcomes.”
When a healthcare organization’s interoperability strategy is incomplete, it can have far reaching consequences for patients. The challenges can include:
- Ad-hoc interventions in patient care
- Ineffective care coordination and member outreach
- Difficult cost containment due to reactive care
- Low patient adherence and care plan personalization
- Poor patient/member retention
When done well, interoperability not only facilitates widespread data collaboration and enables regulatory compliance, but also allows different systems to communicate and collaborate on data more seamlessly. It also enables optimized workflows, patient 360, and ensures more informed business decision-making. And in today’s environment of staffing shortages, cost pressures, and inflation, organizations that adopt a strong interoperability strategy are better positioned to achieve these outcomes and more.
To learn more, download the full Healthcare and Interoperability – Industry-Wide Perspective report or attend our upcoming on Healthcare and Interoperability webinar.

